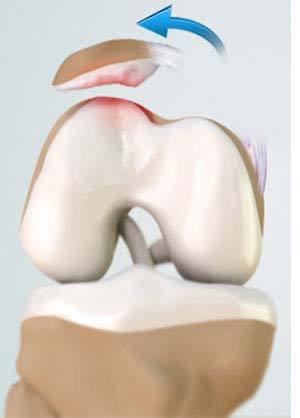
Anatomy of the Knee Joint
The patella (kneecap) is a protective bone attached to the quadriceps muscles of the thigh by quadriceps tendon. It articulates with the femur bone to form the patellofemoral joint. The patella is protected by a ligament called the medial patellofemoral ligament (MPFL), which prevents the kneecap from gliding out.
What is Patellar Dislocation?
Patellar dislocation occurs when the patella moves out of the patellofemoral groove, (trochlea) onto the bony head of the femur. If the kneecap partially comes out of the groove, it is called subluxation; if the kneecap completely comes out, it is called dislocation (luxation).
Causes of Patellar Dislocation
Patella dislocation is commonly observed in young athletes between 15 and 20 years and commonly affects women because the wider pelvis creates a lateral pull on the patella.
Some of the causes for patellar dislocation include a direct blow or trauma, twisting of the knee while changing direction, muscle contraction, and congenital defects. It also occurs when the MPFL is torn.
Symptoms of Patellar Dislocation
The common symptoms include pain, tenderness, swelling around the knee joint, restricted movement of the knee, numbness below the knee, and discoloration of the area where the injury has occurred.
Treatment of Patellar Dislocation/Patellofemoral Dislocation
Your doctor will examine your knee and suggest diagnostic tests such as X-ray, CT scan, and MRI scan to confirm the condition and provide treatment. There are non-surgical and surgical ways of treating patellofemoral dislocation.
Non-surgical or conservative treatment includes:
- PRICE (protection, rest, ice, compression and elevation)
- Non-steroidal anti-inflammatory drugs and analgesics to treat pain and swelling
- Braces or casts that will immobilize the knee and allow the MPF ligament to heal
- Footwear to control gait while walking or running and decrease the pressure on the kneecap
Physical therapy is recommended to control pain and swelling, prevent the formation of scar of soft tissue, and encourage collagen formation. Your physical therapist will extend your knee and apply direct lateral to medial pressure on the knee, which helps in relocation. It includes straightening and strengthening exercises of the hip muscles and other exercises which will improve range of motion.
Surgical treatment is recommended for recurrent patella dislocation. Some of these surgical options include:
- Lateral release: The tight lateral ligaments that pull the kneecap from its groove, increase pressure on the cartilage and cause dislocation are loosened or released.
- Medial patellofemoral ligament reconstruction: The torn MPF ligament is removed and reconstructed using a graft. Grafts are usually harvested from the hamstring tendons, located at the back of the knee and are fixed to the patella tendon using screws. The grafts are either taken from your own body (autograft) or a donor (allograft).
- Tibia tubercle realignment or transfer: The tibial tubercle is a bony attachment below the patella tendon, which sits on the tibia. In this procedure, the tibial tubercle is moved towards the center and held by two screws. The screws hold the bone in place so that it can heal faster and prevent the patella from sliding out of the groove.
These procedures can be performed using an arthroscope.
After the surgery, your doctor will suggest you use crutches for a few weeks, prescribe medications to control pain and swelling, and recommend physical therapy to help you return to your sports activities at the earliest.








